Do you suffer from hay-fever?
Its that time of year again – are you suffering from a runny or stuffy nose, itchy eyes, mouth and skin and fatigue due to lack of sleep. Hay-fever can be debilitating for some people. So what is at the root of it and what can you do?
Hay-fever, sometimes referred to as allergic rhinitis, and other seasonal allergies are basically an imbalance of the immune system. This can be a result of many things – bacterial/yeast/viral infection (these can lurk undetected for years), food intolerances, poor liver function, intensive training without adequate recovery, nutrient deficiencies, ‘stress’ in general, sub-clinical hypothyroidism, disrupted gut microbiome – to name a few. What these all have in common is that they increase inflammation in the body and chronically elevated inflammation has the ability to imbalance the immune system.
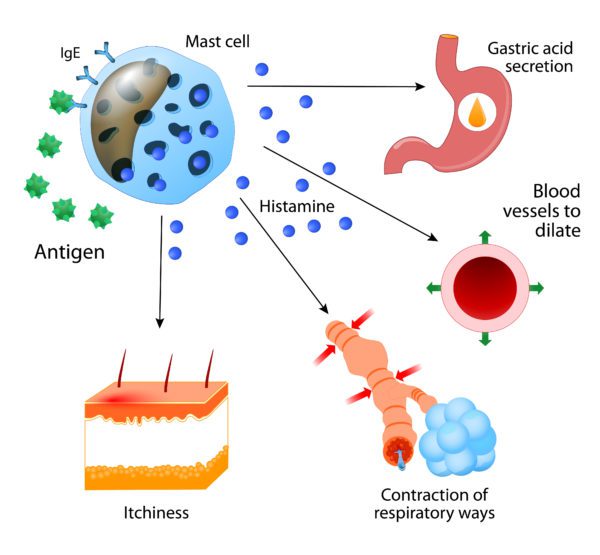
The immune system has a number of different arms to it and it is the adaptive arm, other wise known as TH2, that is typically prominent in allergic type responses such as hay-fever. True allergies set in where your immune system misjudges a harmless protein (known as an allergen) as harmful and develops antibodies against it which are ready to leap into action the next time you are exposed. The antibodies deliver it to a type of white blood cell known as a mast cell and it is these cells, along with basophils and eosinophils, that trigger the release of histamine. Histamine causes vaso-dilation, causing the area to become red and swollen, it can cause a contraction of airways and is responsible for many of your allergic-type symptoms you experience.
The different arms of the immune system all have different roles to play. However, to do their job properly they need to be in balance. Diet, environment, lifestyle and genetics all play a role in determining which arm may become more expressive, along with the overall ‘load’ placed on your body. This goes someway in explaining why adults can develop hay fever later in life as their ‘load’ increases from alcohol, processed foods, stress and nutrient deficiencies, preventing detoxification pathways in the liver from working well, adding to the stress load. Enzymes that breakdown histamine need specific nutrients to work so there is a double-whammy as nutrients are depleted.
So what can you do?
The best, long term solution is to find out what is causing the imbalance in the immune system ie find the root cause. From a functional perspective this involves looking at all the key systems in your body. Depending what else a client may be presenting with, I often suggest starting with a Functional Blood Chemistry panel. This looks at 80 blood bio-markers and uses these to assess possible dysfunction such as:
- Immune Dysfunction – looking at blood bio-markers such as white blood cells, globulin, neutrophils, ferritin, monocytes and serum iron to assess the balance of your immune system.
- GI dysfunction – understanding more about the functional state of your gut helps assess the risk of pathogens, amongst other things. H Pylori, the most common bacterial infection world wide, is known to increase inflammation of gastric mucosa (1). Certain gut bacteria also produce histamine so an imbalance in your gut flora can potentially be increasing your overall histamine ‘load’.
- Thyroid dysfunction – compromised thyroid function alters metabolism and gut motility (2). Reduced gut motility can alter the gut microbiome balance, a key player in immune system regulation.
- Liver Function – compromised liver function means your ability to remove allergens is reduced increasing the body’s overall burden/load.
- Blood Sugar Regulation – imbalanced blood sugar compromises immune function via the insulin/cortisol connection. Every time your blood sugar plummets, cortisol is released, chronically elevated cortisol over a long period of time suppresses immune function (3).
- Adrenal Function – chronically elevated cortisol and high adrenal output has been shown to alter immune function as well as decreasing the body of vital nutrients that are also involved in breaking down histamine.
- Sex Hormones – imbalance in sex hormones alerts one to chronically elevated cortisol and/or imbalanced blood sugar.
- Gall Bladder Function – poor gall bladder function can result in poor absorption of fats, leading to depleted essential fatty acids, key modulators of immune function.
What you can do right now:
- Increase significantly the number of foods containing quercetin in your diet as these inhibit the production of histamine (4). Good sources include onions, tomatoes, broccoli, apples, capers and green tea.
- Reduce the number of high-histamine containing foods in your diet such as fermented foods, beer, aged-cheeses and left-over foods.
- Consider picking nettles to make nettle tea. Nettles arrive just at the right time of the year to ease hay fever discomfort and have been shown to inhibit the body’s production of histamine (5).

- Consider key nutrients in your diet for histamine to be removed properly such as B6, B12, folate and magnesium. Vitamin C has also been shown to support both the innate and adaptive immune system, is a potent anti-oxidant and supports gut mucosal function (6).
- Consider key minerals you may be lacking to support full immune function such as zinc and selenium (shellfish and nuts are good sources).
- Get your vitamin D levels tested (this is done in a Functional Blood Chemistry panel) – vitamin D plays a critical role in the immune system and I find 90% of my clients are deficient.
- Reduce the inflammatory foods in your diet which includes all processed foods, dairy (or at least reduce and alternate with non-dairy), gluten and grains in general (due to high lectin content).
- Assess your intake of essential fatty acids (EFA’s) specifically EPA and DHA which have been shown to modulate mast cell activation (7).
- Pycnogenol has received a lot of attention recently. This is a supplement made from maritime bark extract which is naturally high in proanthocyanidins and bio-flavanoids. Its ability to down-regulate certain key inflammatory pathways is likely to be one mechanism by which it is effective for hay fever along with its reported anti-oxidant properties (8)
If you would like to book a call with Katherine to discuss how she can help click here or fill in the form below.












